Keywords
INTRODUCTION
Right-sided infectious endocarditis (IE) is common in intravenous drug abusers and accounts for 35%-60% of endocarditis cases in this population.1,2 Prior to the increase in intravenous drug addiction in recent decades, right-sided endocarditis was rare and occurred almost exclusively in patients with cardiac malformations.3,4 According to current estimates from large series, only 5%-10% of right-sided IE appear in non-addicted patients.5,6 Definite diagnoses of right-sided IE are exceptional in non-addicted patients without predisposing heart disease. Very few of such cases have been reported in the literature and their diagnosis can pose a significant clinical challenge.7
We describe the case of a man with no prior history of venipuncture, recently diagnosed in our department with tricuspid valve endocarditis in a morphologically normal valve.
CLINICAL CASE STUDY
A 57-year-old man with a history remarkable only for a duodenal ulcer that had been inactive for several years, was admitted for a febrile syndrome (up to 40°C) of seven days' duration, severe generalized joint and muscle pain with significant prostration, reddish dot-like skin lesions on both legs, and inflammation of the left shoulder and elbow. He showed no clinical infectious focus of the respiratory, abdominal, genitourinary or otorhinolaryngological tract. He denied the use of injection drugs or intravenous catheters. He had no alcohol habit, risk behavior for sexually transmitted disease or recent dental procedures. He had no history of rheumatic fever. The patients' clinical history included a small superficial lesion on the left elbow that had occurred 5 weeks before and took several days to heal.
Physical examination showed a temperature of 38°C, fine end-inspiratory crackles in the lower third of both lung fields, a significant limitation in mobility due to intense joint and muscle pain, signs of inflammation in the left acromioclavicular and sternoclavicular joints and to a lesser degree in the left elbow, and multiple dot-like purpuric-petechial lesions on both legs, which were negative on diascopy. All other aspects of the comprehensive physical examination were normal. There were no skin or mucosal stigmata of endocarditis, venipuncture marks, heart murmurs, lymphadenopathy, signs of meningism, or neurological symptoms.
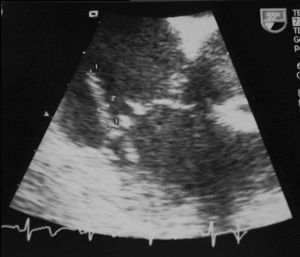
Laboratory analyses disclosed normocytic anemia (10.5 g/dL of hemoglobin), leukocytosis (23 000/μL) with neutrophilia (85%), liver panel alterations with moderate cholestasis (bilirubin, 2.0 mg/dL; alkaline phosphatase, 416 U/L; GGT, 75 U/L), and microscopic hematuria (20 RBCs per field). Bilateral basal parenchymal involvement was seen in the chest x-ray. Serology for human immunodeficiency virus was negative. Oxacillin-sensitive Staphylococcus aureus grew in all four blood cultures and transesophageal echocardiography showed a mobile, 16x3 mm, filiform vegetation in the lateral leaflet of the tricuspid valve, which was morphologically normal apart from this feature (Figure 1). There were no signs of vegetations in the mitral, aortic or pulmonary valves, which were all normal. These findings were corroborated in the follow-up transesophageal study performed 24 days later.
Fig. 1. Transesophageal echocardiogram showing a mobile, 16x3 mm, filiform image inserted in the medial segment of the atrial aspect of the lateral leaflet of the tricuspid valve, consistent with a vegetation.
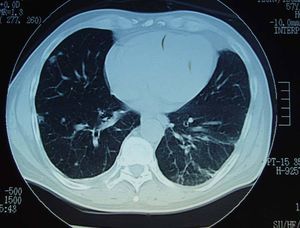
Chest computed tomography (CT) (Figure 2) showed multiple peripheral pulmonary nodules, suggesting septic emboli. No alterations were observed in x-rays of the shoulders and elbows. The diagnosis of native tricuspid valve IE with no clear predisposing condition was established. The portal of entry was not precisely identified, although the left elbow skin lesion described by the patient was considered, even though there was no significant evidence of inflammation. The endocarditis was complicated by asymptomatic pulmonary involvement, anemia, vasculitic purpura, and oligoarthritis, probably due to an immunologic mechanism. Skin biopsy was not performed since the lesions were regressing, and the synovial fluid was not studied because of the small amount.
Fig. 2. Chest computed tomography image showing various small, bilateral, peripheral and subpleural nodules, with cavitation in some cases, suggesting septic emboli. The wedge-shaped opacities with an internal air bronchogram, in which the base is in contact with the pleura, suggest small pulmonary infarcts.
Therapy with parenteral cloxacillin at a dose of 2 g/4 h was started. This treatment was changed to cefazolin after findings consistent with immunoallergic interstitial nephritis were observed (deterioration of renal function with significant peripheral eosinophilia and eosinophiluria, all of which resolved with the change in antibiotic), although there was no histological confirmation. Subsequent challenge study was not considered appropriate. After 6 weeks of specific intravenous antibiotic therapy, blood cultures were negative, the patient was hemodynamically stable and the joint symptoms had resolved completely, leaving no radiologic sequelae.
DISCUSSION
Infectious endocarditis is uncommon in patients who are not drug abusers and have no predisposing heart disease.8 Infection of the right heart valves appears in 5%-10% of all cases of infectious endocarditis1,5,6,9,10 and is almost always associated with intravenous drug abuse, by far the most common predisposing factor, with more than 80% of tricuspid valve endocarditis cases occurring in drug addicts.11 Right-sided IE occurs much less frequently in nonaddicted patients as a complication of permanent intravenous catheter placement, untreated skin or genital infections,10,12,13 or underlying congenital heart disease.4 Tricuspid valve involvement in a patient with no predisposing conditions and a structurally normal heart, as occurred in the patient described, is a clinical rarity in which the diagnosis can be quite complicated.7 No large studies have considered and quantified the frequency and clinical characteristics of this condition.
Generally, isolated native tricuspid valve IE in nonaddicted adults occurs in younger patients, up to the fifth decade of life.8,14 In the majority of cases (70%), there are underlying medical conditions (alcoholism, abortion, colon disease, immunodeficiency, permanent catheters, septic process in the oral cavity, skin or genitals, etc).7,10,12,14 None of these conditions was clearly identified in the case presented.
From the etiologic viewpoint, the pathogen most often isolated is S aureus (although in a smaller percentage than has been described in drug abusers). The portal of entry of the microorganism into the bloodstream is not always determined, as seemed to occur in the present case, where the skin lesion was not conclusive. An inflammatory skin process that might have been the bacteriemic focus of infection was never identified. Nevertheless, the bacteremia is usually endogenous and community-acquired, and the skin is the most common portal of entry, particularly in the case of S aureus.7,8,14 Other sources of infection are the genitourinary tract and the colon.13,14
The clinical presentation invariably consists of persistent fever associated with pulmonary events (generally asymptomatic), anemia and microscopic hematuria, signs that constitute the "tricuspid syndrome," according to the description of Nandakumar and Raju.7 The absence of peripheral stigmata of endocarditis or relevant murmurs in the majority of cases is noteworthy. The murmur of tricuspid regurgitation is usually not detected at the time that the signs and symptoms present, as occurred in the case described. Among the systemic manifestations, the joint, muscle and skin signs that dominate in the picture presented by our patient are not included in the typical clinical data described for nonaddicted patients with native tricuspid valve IE in the main series.7,12,14 This fact makes the case described, in which left heart involvement was ruled out by 2 transesophageal echocardiograms in an interval of more than 3 weeks, even more unusual.
As in any case of IE, the clinical picture, positive findings on blood culture and echocardiography (the gold standard) are the main diagnostic tools in native tricuspid valve IE. In general the prognosis is excellent with medical treatment (specific antibiotic therapy and support have a high success rate) and the development of heart failure is uncommon. Only 25% of cases require valve replacement or surgery. The indications for the latter option are the same as in any patient with IE: failure of antibiotic therapy with persistent fever, or right heart failure.4,10,15 Mortality associated with native tricuspid valve IE is lower than that described for endocarditis in patients with a predisposing condition.8
Correspondence: Dr. J.F. Varona.
Departamento de Medicina Interna.
Hospital 12 de Octubre.
Avda. Andalucía, km 5,4. 28041 Madrid. España.
E-mail: jfva_varona@yahoo.com