Low-density lipoprotein cholesterol (LDL-C) is a strong cardiovascular risk factor, especially for coronary artery disease.1 However, in Spain, there is plenty of room for improvement in increasing the number of patients at very high cardiovascular risk who attain lipid goals.1,2 Recently, our group published the results of the first validation study of the computerized European clinical decision support system (CDSS) specific to lipid-lowering therapy (designated in Spanish as HTE-DLP).3 The study shows that the number of patients who reach the treatment goal of LDL-C < 70mg/dL increases 4.4 times with use of the HTE-DLP by experts in vascular risk.3 The objective of the present study was to assess the theoretical impact on the frequency of coronary artery disease of using the HTE-DLP throughout Spain with the CASSANDRA-REGICOR methodology.4
The CASSANDRA-REGICOR system permits an estimate of the number of fatal and nonfatal coronary events that would occur in the Spanish population in the next 10 years in different scenarios according to trends in prevalence of cardiovascular risk factors. The system uses incidence data on coronary disease and risk factor prevalence from the REGICOR study. Extrapolation to Spain is based on data from the IBERICA study (incidence) and the DARIOS study (risk factor prevalence). The number of coronary events was predicted for 2010 to 2020 in patients aged between 35 and 75 years old. Population projections were provided by the Catalan Statistics Institute (IDESCAT) and Spanish National Statistics Institute (INE). The application enables an assessment of the impact of different scenarios of risk factor prevalence.4
The HTE-DLP is the first CDSS for lipid-lowering treatment developed in Spain (RTA98/09) (Figure). It is based on the 2011 European guidelines for lipid-lowering treatment. Taking into account patients’ cardiovascular risk, comorbidities, and concomitant drugs, the application presents all lipid-lowering therapeutic options for a specific patient, ordered from best to worst according to criteria of efficacy, safety, and cost-effectiveness.3
The mean (SD) value of total cholesterol in HTE-DLP users after 12 weeks was 156.6 (44) mg/dL,3 which in the CASSANDRA-REGICOR system would be equivalent to the effect of the theoretical maximum reduction of 23% for men and 24% for women. To calculate the effect of health costs, a mean cost per coronary event of 14 069 Euros was applied; 87% of this sum corresponds to direct costs and 13% to loss of productivity.5
Use of the HTE-DLP throughout Spain in 2020 would lead to a decrease in fatal and nonfatal coronary events in individuals aged 35 to 74 years of between 5.4% and 7.4% in men and 1.8% and 2.0% in women. This would correspond to a decrease in health costs for coronary disease of between 4.7% and 6.4% (Table).
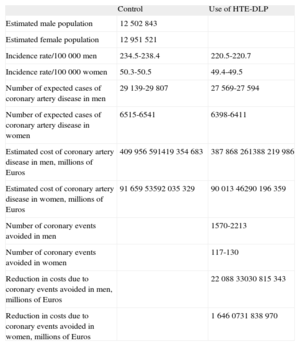
Effect of Using HTE-DLP on the Incidence Rate and Number of Fatal and Nonfatal Coronary Events in Individuals Aged 35 to 74 Years and Health Expenditure Extrapolated to 2020 According to Estimates Based on the CASSANDRA-REGICOR System
| Control | Use of HTE-DLP | |
| Estimated male population | 12 502 843 | |
| Estimated female population | 12 951 521 | |
| Incidence rate/100 000 men | 234.5-238.4 | 220.5-220.7 |
| Incidence rate/100 000 women | 50.3-50.5 | 49.4-49.5 |
| Number of expected cases of coronary artery disease in men | 29 139-29 807 | 27 569-27 594 |
| Number of expected cases of coronary artery disease in women | 6515-6541 | 6398-6411 |
| Estimated cost of coronary artery disease in men, millions of Euros | 409 956 591419 354 683 | 387 868 261388 219 986 |
| Estimated cost of coronary artery disease in women, millions of Euros | 91 659 53592 035 329 | 90 013 46290 196 359 |
| Number of coronary events avoided in men | 1570-2213 | |
| Number of coronary events avoided in women | 117-130 | |
| Reduction in costs due to coronary events avoided in men, millions of Euros | 22 088 33030 815 343 | |
| Reduction in costs due to coronary events avoided in women, millions of Euros | 1 646 0731 838 970 |
HTE-DLP, computerized clinical decision support system for lipid-lowering treatment.
Values presented with upper and lower 95% CI for the mean total cholesterol.
Of the studies published to date on CDSS for lipid-lowering treatment, only the study by Gilutz et al6 in 7448 patients has found a decrease (2.1% in this case), in the number of readmissions to hospital per year for coronary artery disease in the intervention group.
The use of CDSS for lipid-lowering treatment may have an impact not only on direct costs of lipid-lowering medication, which were 19% lower in the case of HTE-DLP for every 1mg decrease in LDL-C,3 but also on indirect costs of these events.
The limitations of the study include the fact that the estimates are approximations to reality based on clinical practice, risk factor prevalence, degree of control, and current demographic trends. In the future, this figure may turn out to be an underestimate, particularly for women, in view of possible variations in the prevalence of risk factors, such as increased prevalence of obesity, hypertension, and diabetes mellitus, and a greater than expected survival of the population, with more individuals aged 75 years or greater. On the other hand, the availability of new drugs and improvements in clinical practice may increase the number of patients who attain their treatment goals, and the findings may be an overestimate. Finally, we should bear in mind that the study data have been extrapolated from the HTE-DLP validation study in a small sample. It is important to highlight that the data used were subject to quality control to guarantee their internal and external validity. However, large prospective studies would be needed in real clinical practice to measure the true effect and safety of CDSS.
In conclusion, the general use in clinical practice of a computerized system for supporting prescription of lipid-lowering treatment may have a positive impact on coronary artery disease and help to optimize the use of health resources.
FUNDINGThe present study was partly funded with a grant from the Instituto de Salud Carlos III to the Cardiovascular Research Network (Red de Investigación Cardiovascular) (Heracles Program, RD12/0042) and AGAUR (2014 SGR 240).
CONFLICTS OF INTERESTA. Zamora and F. Fernández de Bobadilla have intellectual property protection for HTE-DLP.