An 80-year-old man who underwent aortic and mitral valve replacement 2 years earlier had a postoperative episode of atrial fibrillation. The man was anticoagulated for 3 months and had subsequently been maintained in asymptomatic sinus rhythm. Follow-up echocardiography revealed an increased mitral gradient (21 mmHg) and therefore a transesophageal study was performed.
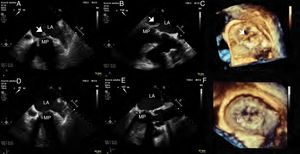
Two- and 3-dimensional transesophageal echocardiography (atrial perspective) revealed a large, elongated mass with chaotic movement toward the left atrium (LA), anchored in a mitral prosthesis (MP) leaflet, together with diffuse thickening and slight restriction of leaflet movement (Figure 1A, B and C, arrow), suggesting prosthetic thrombosis. Endocarditis was ruled out because inflammation markers, blood cultures and PET/CT were all negative.
Due to suspicion of clinically stable obstructive bioprosthetic thrombosis, anticoagulation was selected. However, the patient refused heparin/acenocumarol treatment and repeat surgery. Therefore, dabigatran 150 mg/12 h was prescribed off-label.
Four months later, the mass had disappeared and there remained a discreetly increased gradient and a slight restriction in leaflet mobility (Figure 1D, E and F).
The thromboembolic risk associated with bioprostheses in sinus rhythm after the first 3 months postsurgery is low. Moreover, the cause of the thrombosis was unknown. In the DAWA study, dabigatran was similar to warfarin in patients with atrial fibrillation and bioprosthesis to prevent formation of intracardiac thrombi. However, patients with prosthetic thrombosis were excluded. This case illustrates the efficacy of dabigatran to treat bioprosthetic thrombosis.