To the Editor,
Pacemaker lead malposition is a rare complication, although a few cases have been reported.1,2 The current level of incidence is unknown, probably because of underdiagnosis or underreporting, and treatment is controversial. In some cases, left ventricular (LV) access is through a patent foramen ovale3 or an atrial septal defect;4 in others it is through interventricular septum or sinus venosus type defects,5 atrioventricular membrane perforation6 and right ventricle apex perforation with migration through the pericardium to the LV epicardium.7
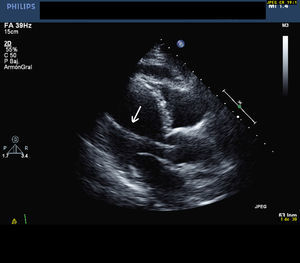
We describe the clinical, electrocardiographic (ECG), X-ray and echocardiographic findings of a 75-year-old woman referred to our diagnostic imaging unit for echocardiography to determine a possible source of embolization, after discovery of basal ganglia infarction in a cranial tomography requested for dizziness. The patient had received a VVI pacemaker implant 9 years earlier, indicated for third-degree atrioventricular block. The ECG showed pacemaker rhythm with complete right bundle branch block morphology. A lateral chest X-ray showed the pacemaker lead was in a posterior location. Transthoracic echocardiography, in parasternal and apical windows, showed left heart cavities were normal, with 60% ejection fraction and mild aortic regurgitation. We determined that the pacemaker lead passed through the aortic valve (Figure 1) and that the electrode had fixed in the mid portion of the left ventricular free wall. No signs of vegetations or thrombus were apparent. We examined the subclavian vessels to determine catheter access and concluded this was located in the artery. The patient was hospitalized for observation and consultations on treatment, and discharged 3 days later following anticoagulation therapy. We decided on conservative management due to her high surgical risk.
Figure 1. Long axis parasternal transthoracic echocardiography. The arrow indicates the pacemaker lead in the left ventricular cavity passing through the aortic valve.
Although pacemaker lead malposition is rare, when it happens it is potentially dangerous due to the risk of perforation and systemic or cerebral embolism. Frequently, diagnosis occurs years after deployment. No agreement exists about treatment, although prolonged anticoagulation therapy is recommended in asymptomatic patients, maintaining an international normalized ratio >2.5. The approach to patient care entails the risk of bleeding, aortic valve trauma and endocarditis. In patients presenting neurologic symptoms, percutaneous or surgical lead removal is preferable and, if not possible, anticoagulation therapy.8 Echocardiography is fundamental in the diagnosis of lead malposition and the identification of structural abnormalities.
To prevent these episodes, we recommend a 12-lead ECG be performed after pacemaker deployment and, if complete right bundle branch block of paced beats is found, we also recommend taking a lateral chest X-ray. If uncertainty remains, echocardiography will determine lead malposition and cardiovascular abnormalities.
Corresponding author: feltesgisela@yahoo.es